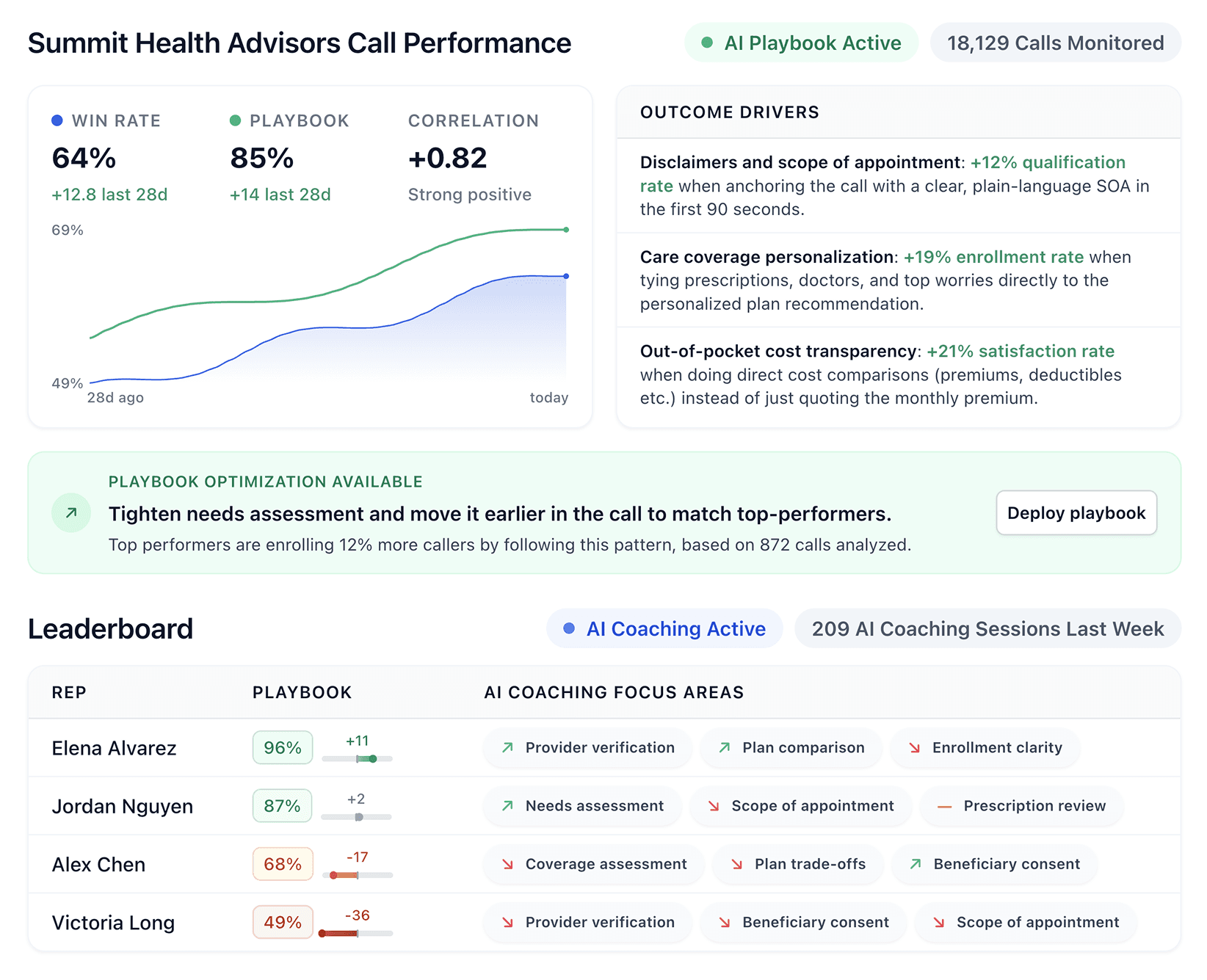
One mishandled call in healthcare can cost you a patient, a referral, and your team's credibility. These healthcare call center best practices cover what every healthcare operation needs, from small practices managing appointment calls to large call centers handling hundreds of patient interactions daily.
Who these practices apply to
Small clinics run lean teams where agents handle scheduling, billing, clinical questions, and follow-ups.
Large call centers (hospitals, insurance companies, and Medicare brokerages) use dedicated teams for each function, with stricter compliance requirements and more advanced technology.
The best practices below apply to both. Scale and tools differ, but the fundamentals stay the same.
How to meet HIPAA requirements in your call center
HIPAA violations carry fines up to $73,011 per incident in 2026, with annual caps above $2 million for repeated breaches.
Beyond fines, a data breach damages patient trust in ways that are hard to recover from. Every healthcare call center needs a clear compliance foundation before anything else.
Encrypt all communications
HIPAA requires protecting patient health information across all channels. Encrypt every call recording, text message, chat conversation, fax, and voicemail.
Verify your vendors have SOC 2 Type II certification and HIPAA compliance before signing any contract. Use platforms that encrypt data in transit and at rest.
Require Business Associate Agreements (BAAs)
Any vendor that handles Protected Health Information (PHI) on your behalf must sign a BAA. This includes your call recording platform, CRM, and any AI coaching tools.
A BAA creates legal accountability and is a requirement under HIPAA.
Control access to patient information
Not everyone on your team needs access to all patient information. Limit access based on what each role requires, and build systems that track who accesses what.
Your access control checklist should include:
Role-based permissions so reps only see data required for their job
Logging every access attempt for audit purposes
Regular log reviews to catch unusual patterns
Immediate access revocation when employees leave the company
Documentation retention for six years (some states require longer)
Former employees with lingering system access cause preventable breaches. A simple offboarding process stops this before it starts.
Train on HIPAA every year
A covered entity must train all workforce members on policies appropriate to their functions. One-time onboarding is not enough because rules change, people forget, and new threats emerge.
Annual refresher training keeps HIPAA top of mind. Include real scenarios your reps face, like what to do if a caller asks you to send information to a family member, or how to verify identity before discussing coverage details.
Document every training session with records of who attended and what topics you covered. You need this when auditors arrive.
20 healthcare call center best practices used by top-performing teams
Most call centers follow the same generic advice and wonder why performance stays flat. These are the practices that actually move the needle.
1. Hire for empathy first (then train everything else)
Here's a truth most hiring managers learn the hard way: you can teach product knowledge, compliance rules, and objection handling. Genuine empathy is a different story.
Healthcare callers are often scared, confused, or overwhelmed. They're navigating a Medicare decision for the first time, processing a difficult diagnosis, or stressed about what something is going to cost.
A rep who actually cares about helping that person will build trust faster, retain patients longer, and generate more referrals than someone just trying to hit a number.
So screen for it. Use role-play scenarios with emotional complexity during interviews. Watch what happens when the caller gets frustrated. That reaction tells you more than any resume.
2. Prioritize active listening on every call
Active listening sounds obvious until you watch a rep cut a patient off mid-sentence to jump to a solution. It happens constantly, and it's one of the fastest ways to lose trust on a call.
Healthcare callers are often anxious before they even dial. When they feel rushed or unheard, they disengage. The conversation falls apart before it starts.
Train your team on habits that actually work:
Repeat back key details before moving forward
Avoid interrupting while the caller is still explaining
Use affirming phrases like "I understand" and "let me make sure I have this right"
Pause before responding to show you've processed what they said
Use the teach-back method: ask patients to repeat key information in their own words to confirm they understood
Drop the jargon; if you need to use a clinical term, explain it immediately
Patients who feel heard are more likely to follow through on appointments, stay enrolled, and refer others. That's not a soft metric. It drives real outcomes.
3. Handle every type of call with a clear process
Not all healthcare calls are the same, and treating them like they are is where a lot of teams go wrong. Each call type needs its own approach.
Appointment scheduling: Confirm insurance information at the start, send reminders, and set expectations for the visit. Fewer no-shows start with better preparation on the front end.
Billing and insurance inquiries: These calls are often emotionally charged. Billing questions can follow scary news. Keep your answers clear, accurate, and free of jargon.
Clinical questions: Route these to licensed clinical staff without hesitation. Agents should never give medical advice. A clear triage protocol protects your patients and your organization.
Emergency calls: Every rep should know how to spot a medical emergency and what to do next. See escalation protocols in item 10.
After-hours calls: A missed call can mean missed care. AI agents or a voicemail system with a clear callback commitment close this gap without requiring overnight staffing.
4. Prioritize patient satisfaction across every interaction
Patient satisfaction is not just about experience, it directly affects retention.
Patients who have a negative experience are three times more likely to switch providers. This means every interaction, especially in your call center, plays a role in whether a patient stays, leaves, or recommends your service.
The factors that move the needle most:
Wait time: Patients who sit on hold too long start to disengage before anyone picks up
First call resolution: Getting a complete answer on the first call matters more than almost anything else
Communication clarity: Patients remember how something was explained, not just what was said
Follow-through: When a rep promises a callback or a resolution, it needs to happen
Short post-call surveys (one or two questions) give you early warning when satisfaction starts slipping. Don't wait for a pattern to become a problem.
5. Implement omnichannel support
Patients don’t think in terms of channels. They just want to reach you in whatever way feels easiest at the moment, whether that’s calling, sending an email, starting a chat, or texting.
The problem is when those channels don’t connect, the experience quickly breaks down:
Patients have to repeat the same information
Reps don’t have the full context and ask the same questions again
Simple issues take longer than they should
And this isn’t just a minor frustration. It goes against what people now expect. In fact, 86% of customers expect conversations to move seamlessly between channels, so they don’t have to start over each time they switch.
Omnichannel support fixes this by bringing every interaction into one place, so if a patient calls after sending an email, the rep already knows what’s going on and can focus on helping instead of catching up.
This matters even more for teams handling Medicare enrollment, insurance questions, or appointment scheduling, where decisions are already stressful and a disconnected experience only makes things harder.
6. Reduce hold times below 60 seconds
The average hold time in U.S. healthcare call centers is 4.4 minutes. The industry target is 50 seconds. That gap is costing teams patients that they never get back.
About 16% of callers hang up before reaching an agent. That's nearly 1 in 6. Every abandoned call is a patient who didn't get help, and in many cases, won't call again.
A few changes make a real difference:
IVR (Interactive Voice Response): Routes callers to the right team without needing a live agent at every step, cutting unnecessary transfers and wait times
VoIP systems: Cloud-based calling scales with your team, supports remote agents, and connects with your CRM and coaching tools
Callback options: Let callers hang up and receive a return call when an agent is free, which cuts abandonment without adding staff
Accurate staffing models: Match your team to actual call volume patterns by time of day and day of week
Track Average Speed to Answer (ASA) and your call abandonment rate every week. If hold times are consistently above 60 seconds, the fix is overdue.
7. Invest in the right call center technology
The tools your team uses every day either make their job easier or harder. The right stack reduces errors, supports compliance, and gives managers real visibility into what's happening across the floor.
Key tools to evaluate:
CRM: Centralizes patient information, tracks interaction history, and cuts time lost switching between systems
Call recording and analytics: Captures every conversation for coaching, compliance review, and quality assurance
Workforce management software: Matches staffing to demand and reduces costly over- and under-scheduling
AI coaching tools: Score calls against your playbook and surface coaching opportunities managers would otherwise miss
Prioritize vendors that integrate with your existing call center platform (Five9, Genesys, etc.) and meet HIPAA requirements out of the box.
8. Use AI voice agents for after-hours and repetitive tasks
About 11% of patient calls come in after hours or on weekends. Most go to voicemail and never get a callback. That's a missed opportunity sitting right in front of you.
AI voice agents pick up where your human team leaves off. They handle:
After-hours lead qualification
Appointment scheduling and confirmations
Initial information gathering
Routine follow-up calls
Your human reps are most valuable in conversations that need real judgment and genuine empathy. AI takes the repetitive work off their plate and gives you 24/7 coverage without a night shift.
9. Focus on first call resolution
First call resolution (FCR) is one of the clearest signals of how well your call center actually works. It measures how often you resolve a patient's issue on the first contact, without them needing to call back.
Every repeat call means your team handles double the volume for the same outcome. Improving FCR cuts repeat calls, reduces handle time, and lifts satisfaction scores across the board.
Track it weekly. When FCR drops, ask why: are reps missing information? Is there a system issue? Is training the gap? The answer almost always points to something fixable.
10. Create escalation protocols for urgent situations
Every healthcare call center will eventually receive a call from someone in crisis. Medical emergencies, mental health situations, and abusive callers all require a clear protocol so reps know exactly what to do without hesitating.
Build your escalation protocol around these elements:
Define when a call escalates to a supervisor or clinical staff
Train reps to recognize language that signals a medical emergency or mental health crisis
Keep a direct line to clinical staff or emergency services ready when needed
Document every urgent situation with timestamps and actions taken
Route high-stress calls to experienced agents who handle pressure well
Review every escalation after the fact to find ways to improve
Not every rep handles high-stress calls the same way, and that's fine. Know who does it best and route accordingly. Regular drills keep everyone prepared before a real situation happens.
11. Build compliance into your operations
Compliance in a healthcare call center isn't something you check off after the call. It belongs inside the conversation itself, woven into how every interaction runs. Your operating procedures should cover:
📋 Compliance requirement | 💡 Why it matters |
Recording disclosures on every call | Confirms the patient understands the call is being recorded |
Delivering required disclaimers | Keeps regulatory messaging consistent across every rep |
Verifying identity before discussing PHI | Protects patient privacy and prevents violations |
Documenting every patient interaction | Creates a clear audit trail for regulators |
Sales teams should track compliance scores alongside conversion rates. A deal that creates a compliance violation doesn't count as a win. Platforms with SOC 2 Type II certification make this easier by creating a verifiable audit trail for every interaction.
12. Cut ramp time with structured onboarding
Healthcare sales reps take 12 to 18 months to reach full productivity, compared to 6 to 9 months in other industries. That extended ramp period can put you at a net loss on a new hire for over a year.
The fix isn't complicated, but it requires intention:
Give new reps immediate access to recorded calls from top performers
Provide real-time coaching during their first live calls
Set clear milestones with specific skills to hit at each stage
Check in often during the first 90 days
AI coaching tools compress this timeline. New reps get instant, call-specific guidance from day one instead of waiting months for their manager to spot a gap.
13. Track metrics that drive performance
Average handle time tells you how long calls take. It doesn't tell you whether the patient got what they needed. The metrics worth tracking go deeper than that.
📊 Metric | 💡 Why it matters |
First call resolution | Shows whether patients got answers without calling back |
Patient satisfaction score | Tracks how patients feel after each interaction |
Compliance score | Tracks how many calls meet regulatory requirements |
Playbook adherence | Shows whether reps follow the process that drives outcomes |
Conversion rate by stage | Reveals where patients or prospects drop off in the funnel |
Ramp time | Measures how fast new hires reach full productivity |
These are the numbers that tell you where to focus coaching and where process changes will have the most impact.
14. Collect feedback after every call
Post-call surveys are one of the simplest tools available, yet most teams underuse them. Keep it short. One or two questions are enough to gather useful feedback without annoying your callers.
Try something like:
Did the agent answer your questions today?
How likely are you to recommend us?
Simple questions give you clear, actionable data on the patient experience.
Track the trends over time. A sudden drop in satisfaction scores can signal a training gap, a process issue, or a new competitive threat. The sooner you catch it, the easier it is to fix.
15. Fight agent burnout before it starts
About 39% of call center organizations say burnout and turnover are their top operational challenge. When you consider what it costs to hire, train, and ramp a new agent, that number makes sense.
Burned-out reps make more compliance mistakes, deliver worse patient experiences, and leave sooner. The cycle is expensive and avoidable.
The best teams get ahead of it:
Automate post-call documentation to cut repetitive admin work
Provide real-time support during difficult calls so reps don't feel alone
Recognize wins publicly and often
Keep caseloads manageable during peak periods
Choose technology that makes the job easier, not more complicated
When reps feel supported and set up to succeed, performance and retention both improve.
For high-volume healthcare sales teams
The following practices are for inside sales teams in healthcare, such as Medicare brokerages, insurance call centers, and home services sales. They build on the foundations above with practices for high-volume, conversion-focused operations.
16. Build playbooks from your actual winning calls
Generic scripts from the internet won't help your team close more deals. One of the most important practices for healthcare sales teams is studying your own top performers to find out what works.
Look for patterns in how your best reps:
Handle objections when a Medicare beneficiary pushes back on price
Ask discovery questions in a specific order
Use phrases that move hesitant callers toward enrollment
Close using language that resonates with your customer base
Document these patterns and turn them into a custom playbook. New hires learn what works in your business instead of theory from a textbook.
17. Score 100% of calls (not random samples)
Most managers review only 5 to 10 calls per rep each week. When agents handle 30, 40, or even 50 conversations a day, most calls never receive feedback.
AI-powered scoring tools solve this gap by analyzing every call against your playbook criteria. Instead of relying on small samples, managers can see where reps follow the process, where they drift, and how performance trends develop across the entire team.
Over time, clear patterns emerge. You can identify which skills need improvement across the team and which reps need targeted coaching, allowing managers to focus their time where it has the greatest impact.
18. Give reps real-time guidance during calls
Post-call feedback helps, but real-time coaching changes the outcome. When a rep hits a tough objection, they need guidance in the moment.
Modern coaching tools provide live prompts based on what the caller says.
If a caller mentions they are on a fixed income, the system can surface guidance like: "Here is how top performers handle this situation."
The rep adjusts and keeps the conversation moving. Over time, every agent benefits from the proven tactics your best performers use.
19. Send coaching notes directly to reps
Managers rarely have time to deliver detailed feedback after every call. That’s why many teams automate the process.
After each conversation, reps receive short coaching notes that highlight what they did well and where they can improve. The feedback stays specific and tied to real moments in the call.
For example: "At 2:34, you missed an opportunity to ask about their current coverage. Try this question next time."
This approach removes much of the manual work from managers while giving reps continuous guidance instead of waiting for the next one-on-one review.
20. Update your playbook continuously
What worked last quarter may not work next quarter because Medicare rules change, competitor offerings shift, and customer expectations evolve.
Build systems that capture new insights as they happen:
Add new tactics to the playbook as soon as top performers discover them
Review call data monthly for emerging patterns
Remove outdated guidance that no longer applies
Your playbook should be a living document, not a static PDF that gathers dust.
Scale your healthcare call center with Alpharun
Healthcare call centers cost $13.9 million per year to run. Every mishandled call, compliance slip, or burned-out rep eats into that investment. Strong healthcare call center best practices help teams protect patient trust and performance.
Alpharun helps teams apply these practices at scale:
Analyzes your calls to identify patterns behind successful conversations
Builds custom playbooks from your top-performing reps
Delivers real-time coaching prompts during difficult calls
Tracks compliance automatically, including HIPAA disclosures and qualification steps
Sends short coaching notes after each call so reps know what to improve
This gives managers better visibility into performance while helping reps handle complex patient conversations with confidence.
Book a demo and see how Alpharun gives your team the best of both worlds: human performance at its peak and AI handling the rest.
Frequently asked questions
What are healthcare call center best practices?
Healthcare call center best practices are the processes, training standards, and technologies that help teams deliver consistent and compliant patient interactions. They include HIPAA compliance procedures, empathy training, performance metrics, and agent coaching.
How do you reduce agent burnout in healthcare call centers?
Healthcare call centers reduce agent burnout by automating repetitive tasks, providing real-time support during difficult calls, and keeping caseloads manageable. Recognition programs and career development paths also improve retention.
What metrics should a healthcare call center track?
Healthcare call centers should track first call resolution, patient satisfaction, compliance adherence, average handle time, and conversion rates. Monitoring these metrics helps managers identify performance gaps and improve patient outcomes.
What is the difference between a healthcare call center and a contact center?
The main difference between a healthcare call center and a contact center is the number of communication channels they support. Call centers focus mainly on phone calls, while contact centers handle phone, email, chat, and text.
What technology do healthcare call centers use?
Healthcare call centers use CRM systems, omnichannel contact center platforms, call recording software, and compliance monitoring tools. These systems help teams manage patient interactions and meet regulatory requirements.